Evaluating the Safety of HBOT for Cancer Patients

Lisa St. John, M.S.
Lisa is our Clinic Director and Founder. She earned her Master's degree from Harvard University, completed a Fellowship at Stanford University, and has spent the last 30 years working in the healthcare field.

Hyperbaric Oxygen Therapy (HBOT) is increasingly considered as a potential adjunctive treatment for cancer patients, sparking interest and debate within the medical community. This blog delves into HBOT in cancer treatment safety, providing a detailed exploration for both patients and healthcare providers.
Understanding Hyperbaric Oxygen Therapy (HBOT)
What is HBOT?
Hyperbaric Oxygen Therapy involves the administration of 100% oxygen at higher than normal atmospheric pressures, typically within a specialized chamber. This process allows the lungs to gather significantly more oxygen than breathing pure oxygen at normal pressures. The increased oxygen levels in the bloodstream are believed to promote healing and combat certain infections by enhancing the body's natural healing processes.
How Does HBOT Work?
In a hyperbaric chamber, the elevated pressure forces oxygen into the body's tissues, even those with restricted blood flow. This increased oxygenation supports cellular metabolism, boosts the immune response, and aids in tissue repair. For cancer patients, the potential benefits include improved wound healing post-surgery, mitigation of radiation side effects, and possibly enhanced effectiveness of some cancer patients' recovery.
Common Uses of HBOT
While initially developed to treat conditions like decompression sickness and non-healing wounds, HBOT has expanded to include various medical applications. In cancer care, it is explored as a complementary therapy to conventional treatments, aiming to alleviate treatment side effects and potentially improve outcomes.
HBOT Research for Cancer Patient’s Safety
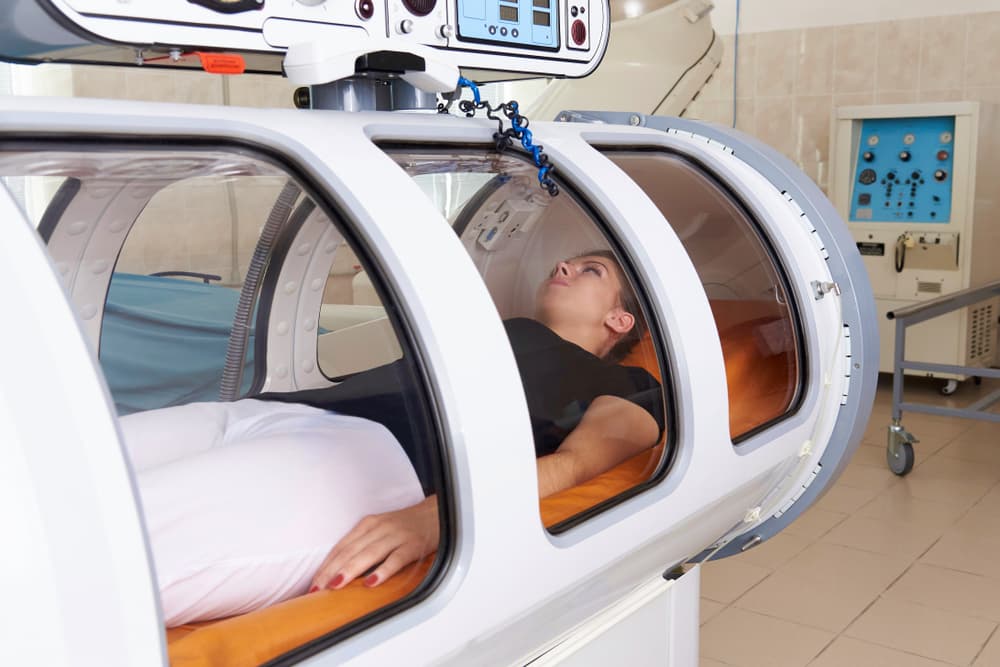
Key Findings from HBOT Clinical Studies
Recent clinical studies have explored the safety and efficacy of HBOT in cancer patients. HBOT shows promise in enhancing healing and reducing side effects like radiation-induced tissue damage. However, its overall impact on cancer treatment outcomes needs further investigation.
A study published in Cancer Research and Treatment reviewed several clinical trials. It found that HBOT could potentially reduce the severity of radiation-induced cystitis and proctitis in prostate cancer patients. However, the study cautioned that more robust, randomized controlled trials are needed to validate these findings across different cancer types and treatment regimens.
Expert Opinions and Guidelines
Medical experts emphasize the importance of integrating HBOT cautiously into cancer treatment plans. Some oncologists advocate its use to manage specific complications, such as delayed wound healing or radiation injuries. Others stress the need for personalized assessments to weigh potential benefits against risks.
Comparative Analysis with Other Therapies
Comparative research underscores HBOT's role as an adjunctive therapy in cancer care. Unlike chemotherapy or radiation therapy, which directly target cancer cells, HBOT focuses on enhancing physiological conditions to support overall treatment effectiveness and patient well-being.
Studies comparing HBOT with other supportive therapies highlight its unique mechanism and potential synergies with standard cancer treatments. However, challenges remain in standardizing protocols and establishing clear guidelines for its integration into oncological practice.
Patient Experiences with Hyperbaric Oxygen Therapy for Cancer Patients
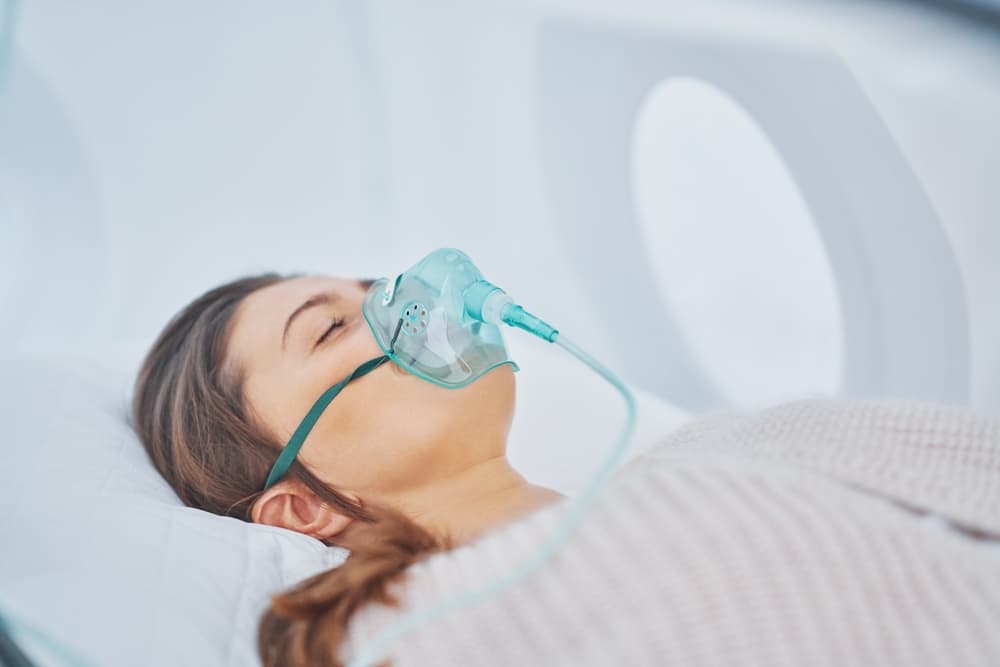
Case Studies of Cancer Patients
Individual case studies provide insights into how HBOT has been utilized alongside conventional cancer treatments. For example, a case report documented the successful management of radiation-induced tissue necrosis in a breast cancer patient following HBOT sessions.
These cases illustrate personalized approaches to integrating HBOT based on patient-specific factors, treatment goals, and medical history. They also underscore the importance of multidisciplinary collaboration among oncologists, radiation therapists, and hyperbaric medicine specialists in optimizing patient outcomes.
Testimonials and Personal Stories
Patient testimonials offer valuable perspectives on the lived experiences of undergoing HBOT during cancer treatment. Many individuals report improved quality of life, reduced pain, and faster recovery from treatment-related side effects after incorporating HBOT into their care plans.
While anecdotal, these testimonials provide anecdotal evidence of HBOT's potential benefits in enhancing symptom management and overall well-being during cancer treatment journeys.
Managing Expectations and Outcomes
Managing expectations is crucial when considering HBOT as part of cancer care. While it may offer symptomatic relief and supportive benefits, it is not a cure for cancer itself. Patients and caregivers are encouraged to discuss potential outcomes, risks, and alternatives with healthcare providers to make informed decisions aligned with individual treatment goals.
Schedule Your HBOT for Cancer Treatment
The safety of hyperbaric oxygen therapy holds promise as a complementary approach in cancer care, offering potential benefits in managing treatment-related complications and enhancing recovery. However, its integration into oncological practice requires careful consideration of patient-specific factors, evidence-based guidelines, and collaborative decision-making among healthcare teams.
For cancer patients exploring HBOT options, Bay Area Hyperbarics provides specialized expertise and supportive care to navigate this adjunctive therapy safely and effectively. Contact us and schedule your appointment.
HBOT for Cancer Patients | Bay Area Hyperbarics
Hyperbaric Oxygen Therapy (HBOT) is increasingly considered as a potential adjunctive treatment for cancer patients. Learn more about it in this blog!
