Hyperbaric oxygen therapy heals diabetic wounds and prevents amputations
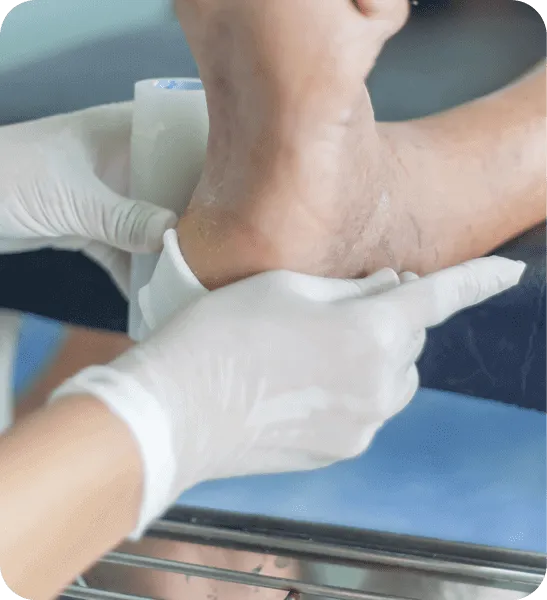
Hyperbaric oxygen therapy heals diabetic wounds and prevents amputations

Why diabetic wounds fail to heal and how oxygen therapy changes the outcome
Diabetes impairs wound healing by damaging blood vessels and reducing oxygen delivery to tissue. Diabetic foot ulcers affect approximately 15% of diabetic patients and are the leading cause of non-traumatic lower limb amputations. When circulation is compromised, wounds become hypoxic and the body cannot produce the collagen, immune cells and new blood vessels needed for healing.
Standard wound care combined with antibiotics often fails to close diabetic wounds because the underlying oxygen deficiency remains unaddressed. HBOT changes this by dramatically increasing oxygen concentration in wounded tissue, even in areas with severely damaged circulation. Medicare, the FDA and the AMA all support HBOT as a proven treatment for diabetic wounds, and numerous private insurance companies cover the condition.
Non-healing foot ulcers and chronic diabetic wounds
Risk of amputation when wounds fail to respond to treatment
Recurring infections in oxygen-starved tissue
Reduced mobility and inability to bear weight

How pressurized oxygen saves diabetic limbs and closes wounds
HBOT addresses the root cause of diabetic wound failure by restoring oxygen delivery and activating the body's healing mechanisms.
Reduces amputation rates by over 50%
Increases oxygen to starved tissues by 1,200%
Stimulates angiogenesis and new blood vessel growth
Mobilizes stem cells for tissue regeneration
Fights infection and supercharges antibiotics
Reduces inflammation and fluid retention
For Providers
Clinical evidence for HBOT in diabetic wound healing
Hyperbaric oxygen therapy for diabetic wounds is one of the most extensively researched and well-supported applications in hyperbaric medicine, with FDA and Medicare approval.
Amputation prevention: Multiple clinical studies demonstrate HBOT decreases the requirement for diabetic amputations by over 50%. A landmark study in Diabetes Care (Londahl et al., 2010) showed significantly higher wound healing rates in diabetic foot ulcer patients receiving HBOT compared to placebo, with particular benefit for patients with adequate perfusion who had failed conventional treatment.
Wound healing mechanism: Diabetic wounds are characterized by tissue hypoxia due to microvascular and macrovascular damage. HBOT bypasses damaged blood vessels by dissolving oxygen directly into plasma at 1,200% normal levels. This hyper-oxygenation stimulates fibroblast proliferation, collagen production, angiogenesis and epithelial cell migration — all essential components of wound closure.
Vascular regeneration: HBOT promotes neovascularization through angiogenesis, growing new blood vessels in the wound bed. This restores long-term blood supply to tissue that was previously cut off, supporting continued healing even after treatment ends.
Anti-infection properties: HBOT is directly bactericidal against anaerobic organisms, enhances the oxidative killing mechanism of leukocytes, improves antibiotic tissue penetration and down-regulates inflammatory cytokines. These combined effects address the chronic infection cycle that prevents many diabetic wounds from closing.
Cochrane Review evidence: A Cochrane systematic review (Kranke et al., 2015) evaluated the evidence for HBOT in chronic wounds and confirmed improved healing rates, particularly for diabetic foot ulcers. The review noted that HBOT increased the likelihood of complete wound healing.
Clinical outcomes at BAH: Bay Area Hyperbarics has treated hundreds of patients with diabetic wounds over 25 years, achieving over 90% wound healing success rates. Our clinic accepts Medicare and most major insurance plans for diabetic wound treatment.
Hyperbaric Treatment of Diabetic Foot Ulcers
Recommendations suggest adding HBOT to the standard of care treatment in patients with Wagner 3 or higher DFU
Diabetic foot ulcers (DFU) occur in approximately 15% of patients with diabetes mellitus (DM) and are commonly located on the plantar weight-bearing surfaces of the foot. Of those patients who develop a diabetic foot ulcer, 6% will be hospitalized for infection or other ulcer-related complications, and 1% of these will require amputation. Complications in patients with diabetes are the leading cause of nontraumatic lower-extremity amputations. This activity discusses hyperbaric oxygen therapy as an effective treatment option.Hyperbaric oxygen therapy for chronic wounds (Review)
Hyperbaric oxygen has been proven effective in healing diabetic foot wounds
Chronic wounds are common and present a health problem with significant effect on quality of life. Various pathologies may cause tissue breakdown, including poor blood supply resulting in inadequate oxygenation of the wound bed. Hyperbaric oxygen therapy (HBOT) has been suggested to improve oxygen supply to wounds and therefore improve their healing.Hyperbaric oxygen therapy facilitates healing of chronic foot ulcers in patients with diabetes
Hyperbaric oxygen therapy healed 61% of patients with chronic diabetic foot ulcers.
Chronic diabetic foot ulcers are a source of major concern for both patients and health care systems. The aim of this study was to evaluate the effect of hyperbaric oxygen therapy (HBOT) in the management of chronic diabetic foot ulcers.Hyperbaric Oxygen Therapy for Diabetic Foot Wounds: Has Hope Hurdled Hype?
Hyperbarics effective in treating diabetic foot ulcers in clinical trials
Hyperbaric oxygen therapy (HBOT) has been promoted as an effective treatment for diabetic foot wounds, and the first controlled trial for this indication was reported (in Diabetes Care) over 20 years ago. Advocates have suggested that the experimentally demonstrated effects of HBOT on improving wound tissue hypoxia, enhancing perfusion, reducing edema, downregulating inflammatory cytokines, promoting fibroblast proliferation, collagen production, and angiogenesis make it a useful adjunct in clinical practice for “problem wounds,” such as diabetic foot ulcers
Diabetic wound patients share their healing stories
Fortunately, this eliminated the tumor. However, it also resulted in a two-inch long non-healing chest wound where the tumor had been.
Fortunately for him, hyperbaric wound therapy healed his chest and skin, so he could return to finish high school, and move on to junior college!
Arun, 17
In addition, his foot remained numb, even where the skin had healed. The hyperbaric wound care treatments Jesus received healed the rest of the sore on his foot, but it also healed the numbness!
Jesus, 57
Her problem was that she developed bedsores on her buttocks that would not heal for months. The sores continued to worsen and got infected so badly that she developed a bone infection (called osteomyelitis).
Her husband was worried about her infections and brought her in for HBO treatment for wounds. After treatment, her bone infection and sores healed completely. She and her husband were very pleased.
Mary Ann, 54
Ankur, 54
Amita, 22
Your path from diabetic wound to complete healing
We design a personalized HBOT wound care protocol coordinated with your physician and diabetes management team.
Comprehensive wound and diabetes assessment
Our medical team evaluates your wound, diabetes management, circulation and previous treatments to design an individualized HBOT protocol with your referring physician.

Daily HBOT sessions in our pressurized chambers
You breathe 100% oxygen in a pressurized chamber for approximately 90 minutes per session. Diabetic wound protocols typically involve 30 to 60 sessions.

Visible wound closure and tissue regeneration
We monitor wound healing progress at every visit. Most patients see visible improvement as new tissue grows, infections clear and wound edges begin to close.

Frequently Asked Questions
Answers to the questions patients and families ask most about hyperbaric oxygen therapy for diabetic wounds and foot ulcers.
Diabetes damages blood vessels, starving wounds of oxygen needed for healing. HBOT delivers 1,200% more oxygen by dissolving it directly into blood plasma, bypassing damaged vessels. This oxygen stimulates new blood vessel growth, mobilizes stem cells, fights infection and activates collagen production — everything the body needs to close wounds that have resisted other treatments.
Save your limb — start healing today
Schedule a free consultation to discuss how hyperbaric oxygen therapy can heal your diabetic wound and help you avoid amputation.

